COVID surge, staffing shortage lead to dire conditions in Wichita ERs, doctors say
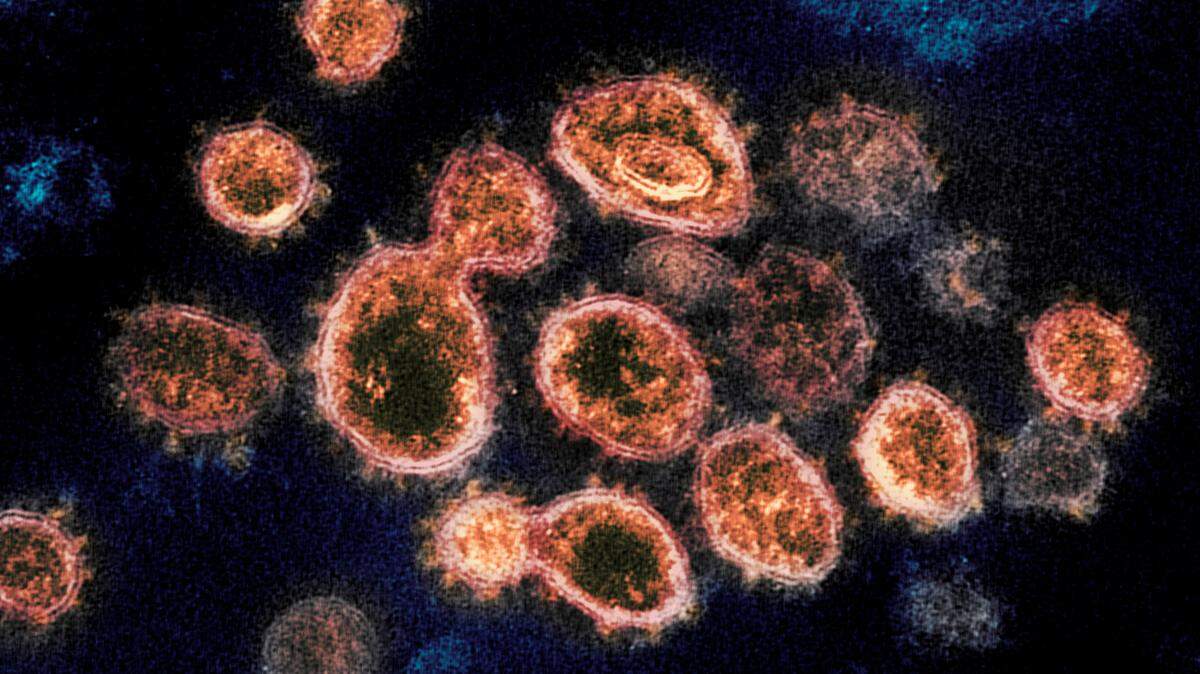
As the U.S. COVID-19 case count reaches its pandemic high, surging illness and a staff shortage are creating dire conditions in Wichita hospitals, according to front-line physicians who say emergency rooms are bursting with COVID and non-COVID patients alike.
“You’ve got people waiting for days in emergency departments, sleeping on the floor or sitting in a chair for two days until a bed becomes available,” said Dr. Tom Moore, the lead physician in Wesley hospital’s COVID-19 unit.
Dr. Mark Mosley, another Wesley physician, said he hasn’t seen such conditions in the 30 years he’s been practicing emergency medicine in Wichita.
“The ER work right now that’s being done, a vast majority is being done in the waiting room,” Mosley said. “Every night, there are 30 to 40 patients — some of them deathly ill — that are being taken care of in a waiting room.”
The problem isn’t that Wesley doesn’t have enough beds. The influx of younger and sicker unvaccinated COVID-19 patients is stretching the hospital’s exhausted staff thin, Mosley said.
Dr. Sam Antonios, Ascension Via Christi’s chief clinical officer, said the surge is also leading to unusually high wait times at St. Joseph and St. Francis hospitals.
“We have nearly 100 patients receiving care for COVID-19, straining our staff resources and the number of beds we have open for other types of care,” Antonios said in an email.
‘When they get sick, they just crash’
Although the highly contagious omicron variant is now the dominant COVID-19 strain in the U.S., the delta variant is still what’s driving hospitalization in Sedgwick County and across the state.
Dr. Chloe Steinshouer, a pulmonary and critical care physician at Wesley, said holiday gatherings and a disregard for public health guidelines have triggered a surge that threatens to overwhelm already critically strained hospitals.
According to Sedgwick County’s most recent weekly hospital update, Wesley and Ascension had a combined 181 COVID patients on Tuesday, 66 of whom were in ICU. And the Kansas Department of Health and Environment’s COVID dashboard reports there were 702 cases in Sedgwick County on Dec. 27, the highest number of the year.
“The surge that we’ve seen since Thanksgiving has everything to do with delta being a highly infectious and highly virulent or dangerous variant,” Steinshouer said.
Wesley officials say at least 95% of their COVID-19 patients are unvaccinated against the virus. According to the New York Times vaccination tracker, 50% of eligible Sedgwick County residents are fully inoculated.
“These are younger people who had previously been healthy and are very, very sick,” Steinshouer said.
The COVID-19 treatments physicians have at their disposal work well when administered early, but few patients realize they’re infected in time for the drugs to be effective, Steinshouer said.
She said she’s seen the same story play out over and over again in Wesley’s intensive care unit. Patients’ lungs fill with fluid and stiffen rapidly.
“People get sick faster, and when they get sick, they just crash,” Steinshouer said.
“You’re looking at a constant flood of patients coming in over and over with something that you can’t fix.”
Once a COVID-19 patient is sick enough to be hospitalized, there are no highly effective treatments that guarantee survival or the absence of long-term complications.
The futility of the situation has taken its toll on hospital staff, even the doctors and nurses who confront death every day in the ICU, Steinshouer said.
Staff exhaustion, abuse
Mosley stressed the grave nature of the staffing shortage gripping the region’s hospitals and breaking the “supply chain of human resources” needed to deliver timely healthcare.
High-paying jobs in states hit even harder by the virus have lured many intensive care nurses away from Kansas.
Steinshouer said some who have been fighting the virus on the front lines since early 2020 are leaving the field altogether due to exhaustion and trauma.
“I have never seen death on this scale, and I don’t know anybody that I work with that has seen death on this scale,” Steinshouer said. “It’s outside of living memory for a single disease to take up 50% of your ICU beds.”
But beyond the ever-present sickness and death, she said she and other staff have become accustomed to having their motives questioned and even being verbally abused by patients’ families.
“You’re putting yourself and your family in danger to take care of these people every day, and you have somebody questioning whether you’re trying hard enough to take care of them,” Steinshouer said. “And you’re working 12-, 14-, 20-, 24-hour days consistently and constantly for nearly two years.”
Moore, the lead physician on Wesley’s COVID unit, said misinformation has fomented a deadly combination of distrust and hostility.
“We’ve got people who have refused to get the vaccine, who come to the hospital, don’t believe that people in the medical profession are there to help them — believe we’re there to kill them, that somehow we’re on the take and we want to make sure we give them expensive, harmful medications instead of cheap, easy cures,” Moore said.
“They’ve been misinformed. They’ve been led astray by charlatans who stand to gain money and fame by peddling nonsense, and unfortunately leading directly to the deaths of people.”
Mosley said the pandemic is testing the limits of empathy and altruism in healthcare professionals who devote their lives to caring for patients.
“The people in the trenches, even some of the most optimistic, energetic, give their life for the mentally ill, homeless, poor, disadvantaged, they’ve gone from tired to angry,” Mosley said. “That’s a bad place to be, because the entire healthcare industry works off of empathy, and when anger starts to replace empathy, you have a crisis in healthcare that’s even bigger than staffing.”
Looking forward to 2022
Mosley said he fears what will happen when local emergency rooms get their annual influx of patients suffering from seasonal illness and injury, including ice-related fractures and respiratory syncytial virus (RSV) in babies.
“When bad weather hits, we have people breaking ankles right and left on the first week of ice, and we have to do conscious sedation, which requires two nurses to get people’s bones back into place,” Mosley said.
“That’s not going to happen. We don’t have the people to do that. I don’t know what’s going to happen when you have someone with a bone sticking out of their leg and it’s going to take four hours to find an available nurse to get that bone back into place.”
Antonios, Ascension Via Christi’s chief clinical officer, said it’s imperative that people protect themselves against the spread of COVID-19 to mitigate the post-holiday hospitalization surge officials are already expecting.
“For everyone’s sake, we strongly urge people to weigh the risk vs. the benefit in making their holiday plans and to get vaccinated for COVID-19 and the flu if they are not already done so,” Antonios said. “We also are encouraging everyone to wear a mask if they are out in public.”
Steinshouer said she knows people want the pandemic to be over, but there will be no easy way out of the woods.
“There’s been so much focus on any individual mechanism being the key to solving or fixing or curing COVID,” she said.
“You stack multiple, imperfect measures on top of each other to optimize them.”
Prevention is the best way to keep everyone safe, she said. Once a critically ill patient makes it to her in the ICU, it may be too late to save their life.
“Vaccination is by far the best because it teaches your body what to do so that if you do get exposed, I don’t have to see you,” Steinshouer said.
This story was originally published December 31, 2021 at 5:03 AM.