Kansans with COVID-19 dealing with the effects weeks, months later
Randy Mousley, a retired USD 259 educator and former president of the United Teachers of Wichita, started to have gastrointestinal issues at the beginning of April.
His wife, Carolyn, already had a cough and headache and felt fatigued. When their conditions didn’t improve, the couple went to be tested for COVID-19. The tests were positive. It had been roughly two weeks since the symptoms started — the amount of time once thought to recover from the virus.
It can be hard to tell the difference between flu and COVID-19 based on symptoms alone, according to the Centers for Disease Control and Prevention (CDC).
But new data shows how different the virus is from influenza and how much longer it can take people to recover. And, despite early reports about older people having a harder time recovering from COVID-19, data is starting to show younger people also struggling to recover.
One-fifth of people ages 18-34 who were infected but not hospitalized, and who had no severe medical conditions, had not returned to feeling normal two-three weeks after testing positive, according to a study published by the CDC. Among all adults, 35% reported they had not felt back to normal two-three weeks after testing positive.
“In contrast, over 90% of outpatients with influenza recover within approximately 2 weeks of having a positive test result,” the CDC wrote.
Effects of coronavirus
For people with COVID-19, the severity of the after-effects varies.
Randy Mousley, 60, feels more fatigued performing normal activities such as mowing the lawn. He also has been prescribed medicine for hypertension, which he suspects is a result of COVID-19. Carolyn Mousely, a retired hair stylist, has numbness in her legs, heart palpitations and a dry cough that she plans to see a physician about. Her symptoms also developed since contracting COVID-19. Neither had any underlying health issues.
“There are things that have manifested that we did not have medically before our infection, but not as bad as other people,” Randy said.
Randy said their symptoms have been minor compared to some people’s symptoms they read about on Survivor Corps, a Facebook group with more than 95,000 followers that they joined. A COVID-19 survivor started the group to give people a place to share their stories and promote them donating plasma to help others recover.
Multiple ER visits and a tracheotomy
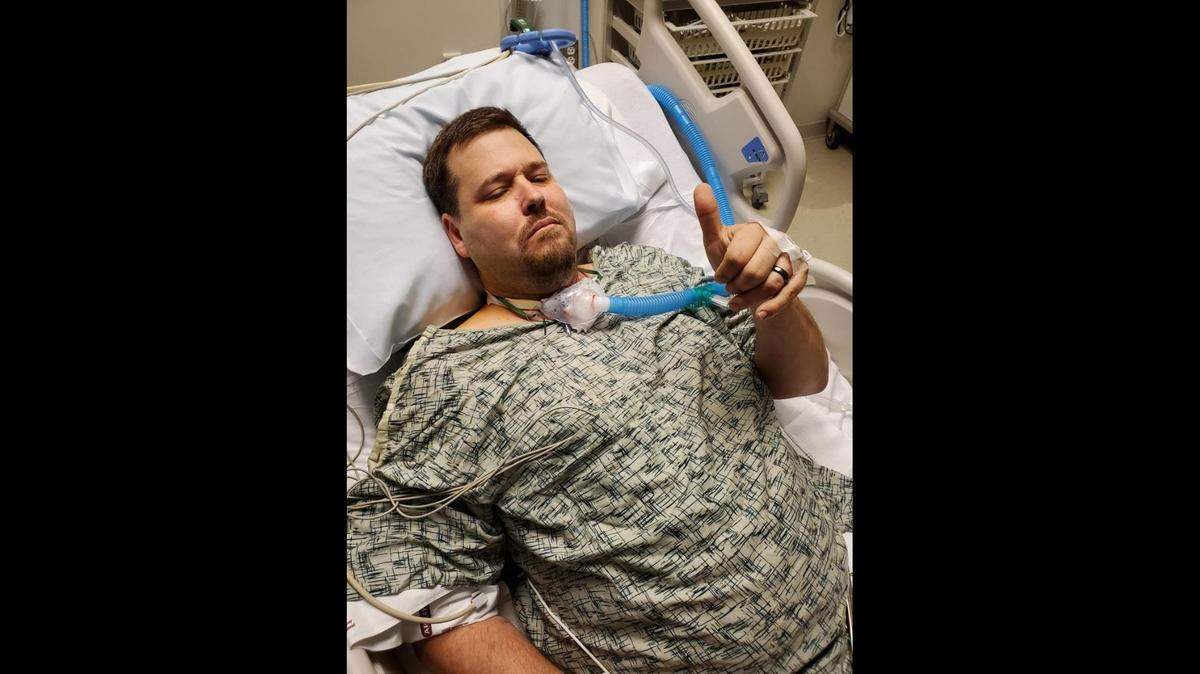
Anil Gharmalkar of Oswego is one of the many people who have shared their story in the group. The truck driver has had multiple emergency room visits and a life flight from Labette Health in Parsons to the University of Kansas Medical Center in Kansas City.
Before the life flight, Gharmalkar, who has Type 1 diabetes, had an hour to contact family and friends. The 41-year-old used that time to make sure his wife had all the necessary information to run their trucking business.
“Whether I was going to live or not was kind of in question at the time,” Gharmalkar said.
Gharmalkar said he had to have a tracheotomy because of the inflammation caused by COVID-19 and irritation from a ventilator tube resting on his throat. The ventilator was a last-ditch effort to save his life, Gharmalkar said.
He’s currently on steroids to keep the inflammation down, but it’s possible he that he’ll live the rest of his life breathing through the tube, though he’s considering a procedure to create a new breathing airway.
Long-hauler study
Dr. Natalie Lambert, an associate research professor at Indiana University School of Medicine, uses social media to collect data about what patients experience. For her research into the long-term effects on COVID-19, she came across a large cohort to study in the Survivor Corps Facebook page.
In collaboration with Survivor Corps, Lambert had a survey posted in the Facebook group. The results were published in a study called COVID-19 “Long Hauler” Symptoms Survey Report.
“Everyone tells this story that it is the flu, but what type of flu gives you memory problems ... It’s not a flu as we can think of it,” Lambert said.
Out of the 10 most reported symptoms the survey participants noted, four show up as symptoms the CDC recognizes — although the CDC’s synopsis of the virus could change as more data becomes available.
The CDC lists 11 total symptoms that go hand-in-hand with the virus. Long-haulers listed 98 symptoms in the study.
Long haulers described 26.5% of the symptoms as being painful.
The most-reported symptom had 1,567 responses, meaning that is the minimum amount of people who took part in the survey — Lambert said it’s likely much higher. Fatigue was the No. 1 response, followed by muscle and body aches, shortness of breath or difficulty breathing, and difficulty concentrating or focusing.
The biggest takeaway from the study was the number of long-haulers who reported neurological issues after the virus was out of their system, Lambert said.
Lambert also took the symptoms and categorized them by the corresponding body part they affected. The brain was No. 1 with 6,505 responses, followed by body, lungs and muscles. The lowest responses for symptoms included blood, thyroid and urinary tract.
“The virus doesn’t look the same for any two people, and we don’t know why that is yet,” Lambert said.
The No. 1 response under the brain category was difficulty concentrating or focusing.
Symptoms a month later
The difficulty concentrating or focusing and difficulty breathing are the main symptoms felt by 29-year-old Abby Hoffman, who still notices them more than a month after testing positive.
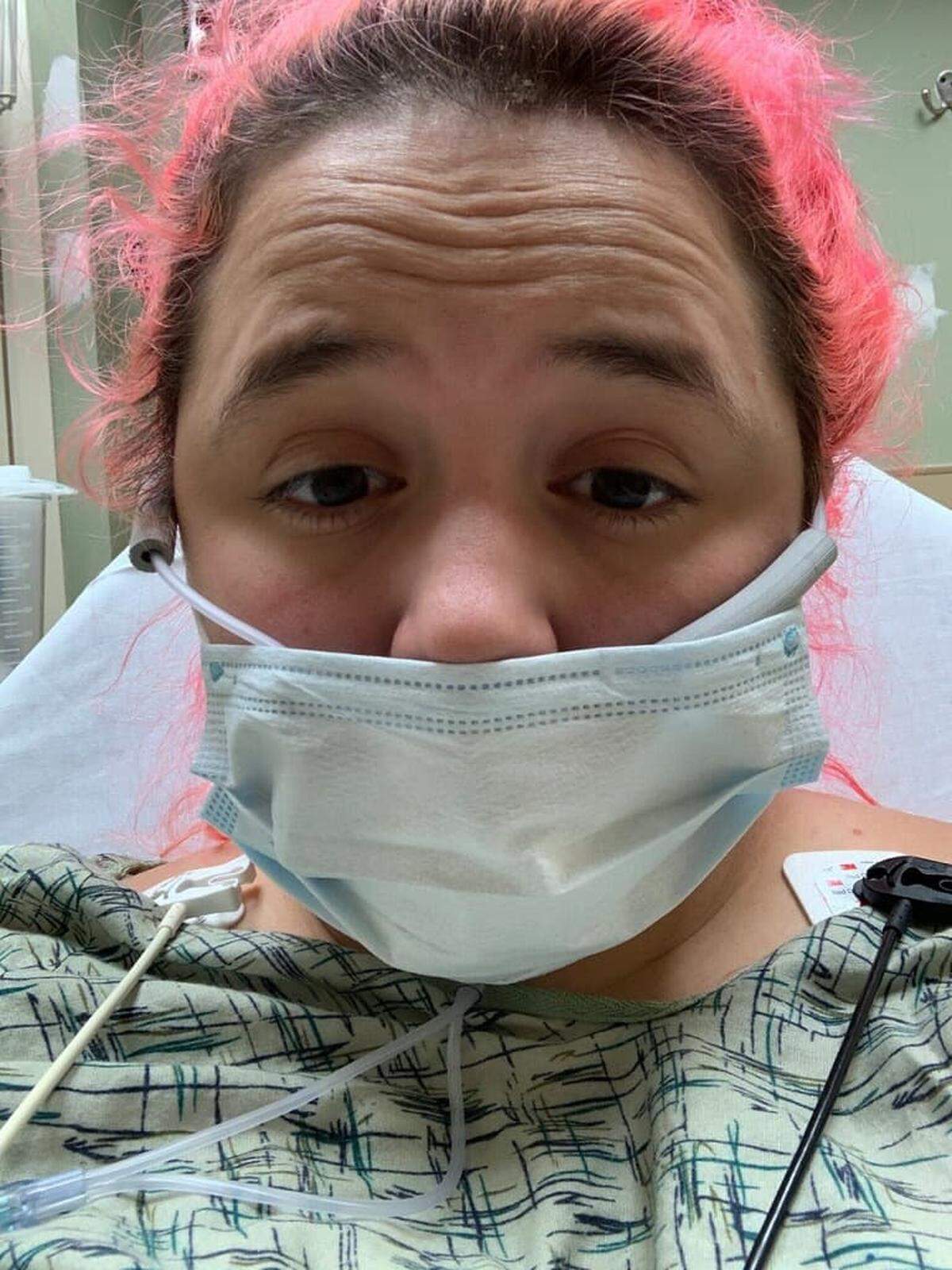
The Lawrence High School English teacher and leisure runner exposed a family member to the virus before testing positive, but the family member didn’t end up with as severe of symptoms as Hoffman.
At the beginning of July, Hoffman thought it was a sinus infection, but after more than a week of trying to sleep it off while taking Mucinex, Hoffman went to the emergency room. Medical staff administered a rapid COVID-19 test, which came back positive.
Hoffman was admitted to the intensive care unit and was hospitalized for six days before being well enough to be discharged. Hoffman was sent home with an inhaler.
In a follow-up appointment, a primary care doctor told Hoffman to continue using the inhaler as needed. Daily walks require a puff to help with breathing.
“I asked my doctor … ‘how long is this going to be?’ ” Hoffman said. “And she looked at me and she said, ‘Abby, I don’t know.’ ”
The anxiety and uncertainty about recovery contributed to Hoffman starting teletherapy.
Anxiety is the No. 3 reported symptom that falls under the brain category in the long-hauler study.
COVID damage to hearts
Lung and breathing difficulties from the virus are the biggest killers followed by deaths from heart complications, according to Dr. Bassem Chehab.
The Ascension Via Christi medical director for the structural heart program said those heart-related deaths happen usually within 14 days of symptoms appearing, but he is seeing people come back with severe heart damage six to eight weeks after symptoms start.
Like the flu, COVID-19 can cause long-term effects on the heart, except heart conditions from COVID-19 are “more pronounced, more significant and more deadly” than those from flu, Chehab said.
He has seen damage to hearts from COVID-19 to be at least 20-30% higher than that from the flu. Using what medical professionals know from heart damage in other diseases, including the flu, Chehab said the COVID-19 damage on the heart can take decades to heal or never heal at all.
“So it’s not just age anymore, it’s not just the elderly at risk. Everyone is at risk and the problem is you cannot predict who is really going to crash and burn on you from the heart,” Chehab said. “There is no formula yet. We don’t know. So the fact that you are younger by no means protects you at all from congestive heart failure and heart damage from COVID.”
Limited data in the data-driven medical field also means healthcare workers don’t have a consensus on how to treat patients.
“Unfortunately there is still many things we do not know or understand about the intermediate and especially the long-term effect of COVID-19 on the population,” Chebab said in a follow-up text.