As coronavirus surges, Kansas and Missouri hospitals apply early lessons to new patients
When the coronavirus first arrived in Kansas and Missouri, doctors feared large numbers of patients would need ventilators. No one knew what drugs might be effective. They saw what was happening in hot spots like New York and prepared for the worst.
Four months later, if you contract COVID-19 and need to be hospitalized, your experience may be different than those earliest patients.
A combination of clinical lessons learned and better data is giving doctors more and better weapons to use against COVID-19. Interviews with hospital leaders and front line providers illuminate how the medical profession in Kansas and Missouri has adapted to fight a cunning foe.
Steroids, the promising antiviral Remdesivir and techniques as simple as turning patients over to help them breathe, are now part of the arsenal when battling the most severe cases of COVID-19.
“We’ve gotten better at treating this disease,” said David Wild, an anesthesiologist and vice president of performance improvement for the University of Kansas Health System.
Hospitals in Kansas and Missouri are putting those lessons to use as they brace for a new onslaught of patients as the virus surges. With both states recording hundreds of new cases each day — and many more cases likely going undetected -- doctors fear resources will soon be strained.
The number of COVID-19 patients in Kansas hospitals, for instance, now exceeds the state’s spring peak. On Monday, 373 patients were currently admitted compared to a high of 295 on May 12.
But fewer people are dying. The majority of KU’s COVID patients have survived. Since the first week in March, the KU hospital system has discharged 350 COVID patients. About a couple dozen patients died. The last death came on June 26.
“We saw 80 percent of our deaths before June, in March, April and May,” Wild said.
To be sure, COVID-19 is a serious virus and much remains unknown about its long-term effects. Doctors stress the importance of masks, social distancing and other precautions to prevent infection and that no one should be dismissive of its dangers.
And even the latest advances may be overwhelmed by a wave of patients. In Kansas City, officials at Truman Medical Centers/University Health have resurrected surge plans created in the early months of the pandemic because hospitalizations there are climbing. Ascension Via Christi in Wichita is also revisiting its surge plans as COVID-19 hospitalizations rise.
Some data is encouraging. The Missouri Hospital Association reports that the average length of stay has declined from 14.6 days on March 20 to 6.3 days on May 20. The percentage of patients in ICU and on ventilators has declined as well.
The death rate for hospitalized COVID-19 patients in Missouri has declined slightly: 20.7% on March 20 to 19.1% on May 20.
Nationally, some data suggests patients are getting better faster, according to Todd Rice, associate professor of medicine in the Division of Allergy, Pulmonary and Critical Medicine at Vanderbilt University in Nashville. Estimates are that patients on average leave the hospital three to five days faster and mortality is falling, he said.
Overall, care and patient outcomes in the United States are “considerably better” now than four months ago, Rice said.
“I think we’ve done some phenomenal learning. We’ve seen science work at the fastest pace we’ve ever seen science work and we’ve learned lots of stuff, and with that we’ve only gotten better and better and better at taking care of these patients,” Rice said.
“And because of that we have better outcomes and patients are doing better and hospital stays are shorter and people are dying less frequently.”
Ventilator alternatives
The early weeks of the pandemic raised widespread fears of ventilator shortages across the United States. The oxygen levels of people with coronavirus were plummeting to dangerously low levels, prompting physicians to hook patients up to machines that forced air into their lungs.
At Ascension Via Christi in Wichita, doctors tried to bring in machines used for student training. And they looked at ways to bring outdated machines, perhaps 20 to 30 years old but still in good working order, into their lineup, said Don Carden, the hospital’s director of respiratory care.
“We did not have experience in Kansas treating COVID-19 initially, so we were attentive to any news, especially from other health care providers anywhere in the world as to what they were learning. And the message we got very strongly was that these patients came into the ER, they could deteriorate very rapidly,” Carden said.
“The recommendation was to intubate as quickly as you could pretty much,” he said. “We anticipated that would be our treatment, too.”
A study published in May by Critical Care Medicine found 35.7% of critically ill coronavirus patients who were placed on a ventilator died. Researchers studied outcomes at ICU facilities in Atlanta between early March and late April.
But soon after Ascension Via Christi began treating coronavirus patients, they decided to shift their approach.
The hospital turned to proning — laying patients on their stomachs instead of their backs.
“As simple as that sounds, that actually makes a very big difference in the lung,” Carden said.
While being placed on your stomach may sound uncomfortable, patients in a prone position often have an easier time breathing, making it less likely they’ll need a ventilator. Patients in less serious condition are often able to turn themselves over. For those in worse shape, a whole team may help coordinate the roll, Carden said.
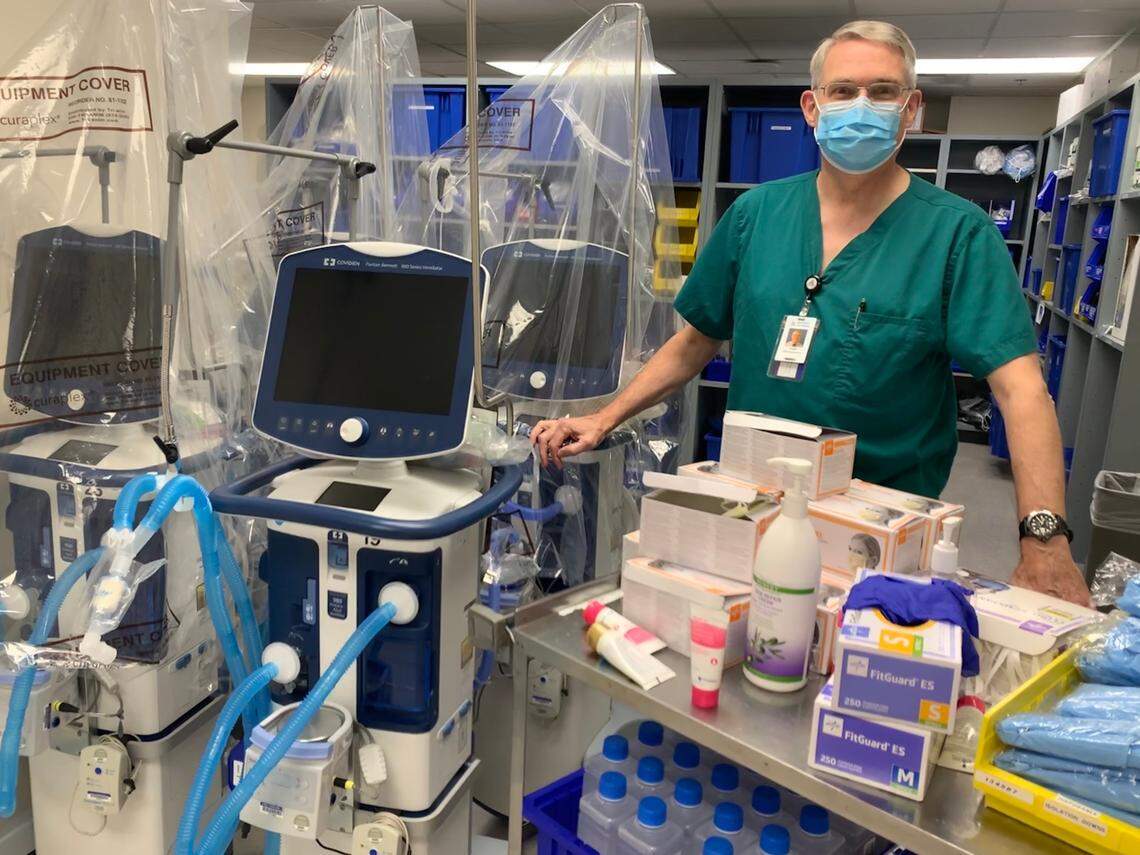
At the beginning of the pandemic, concerns existed nationally that certain ways of delivering oxygen to patients other than ventilators — pressurized masks, for example —might increase the risk of transmitting the virus to those taking care of them, Rice said.
“Now we have good data that that doesn’t actually spread the virus more and they are effective methods for delivering higher levels of oxygen that we can deliver without having to put a patient on a ventilator,” Rice said.
In Kansas, ventilator use has remained relatively stable during the pandemic. After a peak of 34 coronavirus patients on a ventilator on May 7, the number fell and didn’t exceed 20 during June. The number has begun creeping up again, however, and was 28 as of Tuesday.
At the same time, the percentage of ventilators available has slowly fallen since the start of April. On April 1, 95% were available, according to state data. The percentage stood at 83% on Tuesday.
Meanwhile, while Kansas hospitals aren’t short of ventilators, the use of intensive care unit beds is rising. The percentage of ICU beds available has fallen from nearly 75% in early April to 36% this past week, according to data from the Kansas Department of Health and Environment.
Since the start of June, the number of ICU beds in use by COVID-19 patients has risen from about 25 to 112 on Tuesday.
Drugs, plasma promising
As the pandemic has progressed, doctors are also growing more confident about what drugs may help. While COVID-19 may be widespread until a vaccine is developed, drugs will be key in treating symptoms and lessening the severity of the disease.
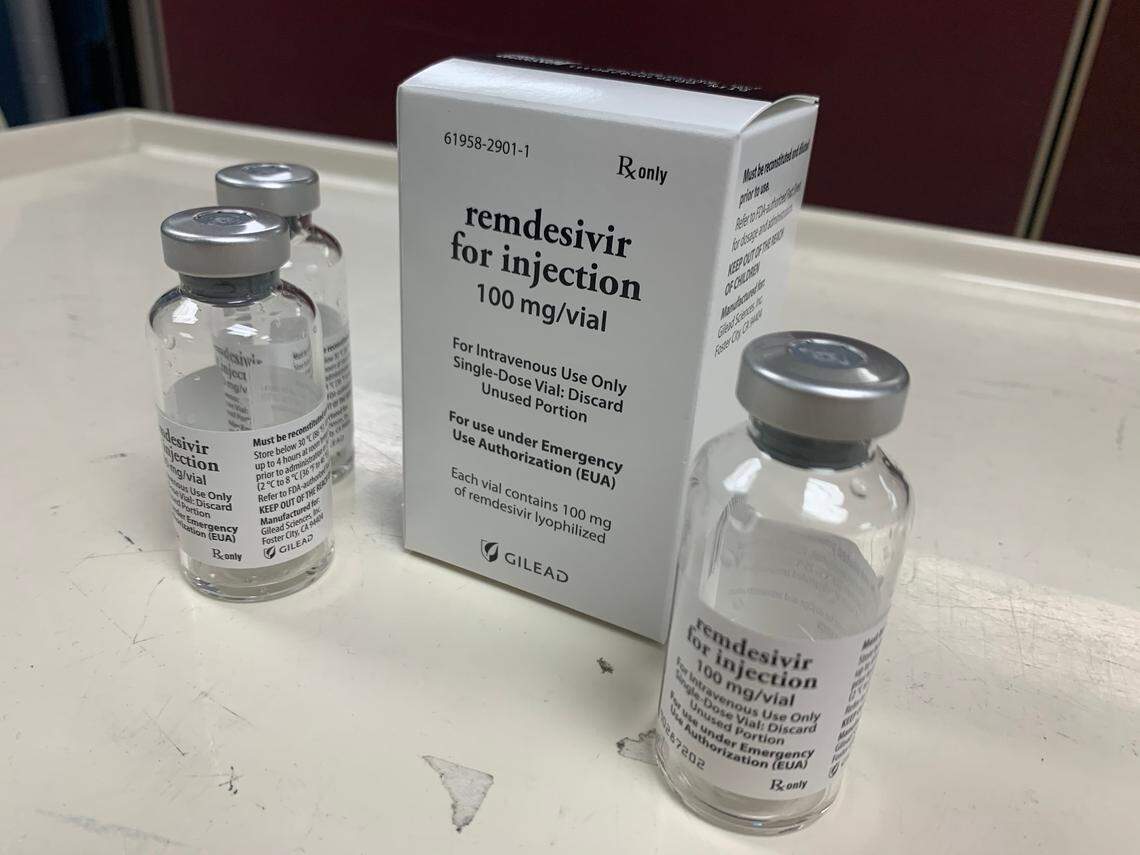
One of the most promising to emerge so far is Remdesivir, an antiviral previously studied for possible use against Ebola. A government trial found the drug accelerated recovery from COVID-19 by 31 percent.
“Every patient that qualifies and needs to be treated with Remdesivir, they’re being treated with that,” Kansas Department of Health and Environment Secretary Lee Norman said on July 8.
In Wichita, Ascension Via Christi is also using plasma from recovered COVID-19 patients. As of Thursday, 58 patients had participated as part of a Mayo Clinic-led study, with 30 of the patients receiving infusions in the past three weeks.
“The (medicines and equipment) we now have to treat COVID infections, which includes convalescent plasma and antiviral medication, have made a big difference. We have seen patients improve quicker and avoid the need for a ventilator because of these therapies,” Maggie Hagan, the hospital’s medical director of infection prevention and control, said in a statement.
Despite advances in care, doctors and scientists are constantly learning more that will continue to shape how patients are treated. Little is known, for instance, about the long-term effects of the virus because it is so new.
Wild, the KU anesthesiologist, said some patients are requiring admission to the hospital a second time. Some have scarring of the lungs and other issues that lead to chronic conditions and multiple hospital visits.
“So part of the story is younger patients needing less time in the hospital when they are acutely infected, but we don’t really know the whole story about how COVID is gonna impact people in the long-run. And we are seeing that. And we are not unique,” Wild said.
‘We have an option’
Despite advances in care, problems are simmering that could still create significant challenges.
As fall approaches, mild illnesses such as the common cold — which share symptoms with COVID-19 — could leave people wondering whether they have a normal ailment or coronavirus. Uncertain of what they have, people may quarantine out of caution.
That process, repeated over and over again, may make carving out some semblance of normal life next to impossible.
“We don’t want to miss a COVID case, right? So we’re ordering these tests on these people who probably have colds, but you don’t want to miss it because they have contacts and such,” said Chad Johanning, a Lawrence doctor and president of the Kansas Academy of Family Physicians.
But the amount of time it takes to get test results from commercial labs is growing. As cases surge nationally, the turnaround time has grown to five to seven days, Johanning said.
Seven days is half of the possible incubation period of the disease. And if a test result is positive, it’s very difficult to conduct contact tracing so long after exposure. Johanning called the lag time for test results the “biggest holdup” right now.
“My personal opinion is there’s no way we ever get ahead of this if our turnaround time is three days or more. There is just no way,” Johanning said.
The more coronavirus spreads within communities, the more likely hospital workers and other medical professionals are to become infected, said Cindy Samuelson, spokeswoman for the Kansas Hospital Association. Rather than picking up the virus at work, doctors and nurses may face the greatest risk at home with family and when they’re out and about.
“They too, like us all, are only as strong as their weakest link,” she said.
Hospitals have renewed their focus in recent weeks on the importance of masks, social distancing and limiting mass gatherings, Samuelson said. That’s also been echoed by actions in Kansas by Gov. Laura Kelly to mandate mask use.
Whether residents adopt these measures will determine whether Kansas and Missouri hospitals are stretched thin, doctors say.
“In many ways we became a victim of our success. We saw how well it worked and we said, ‘Hmm, OK. Things got better.’ And we kind of got a little more relaxed and now things are getting worse,” Wild said.
“It’s not like there’s no option here. We have an option. We really do,” he added. “And it’s not an option that requires hundreds of thousands of people in Kansas City in the hospital, and hundreds in the ICUs. So there’s hope there.”
The Eagle’s Katherine Dynarski contributed reporting
This story was originally published July 24, 2020 at 5:02 PM.