Bigger cities face organ donation shortage. So they plan to take them from KC area
U.S. senators from Kansas and Missouri are leading a fight over how transplant livers are distributed, pitting more rural states with high donation rates against patients on the coasts who say they have to wait too long.
The fight is over changes that will take effect April 30, allowing people who are sicker to get a better chance at a matching liver, even if they live as far as 500 miles from where it was donated. Right now the change only applies to livers, but it could become a model for other organ transplants as well.
The change, approved by the Organ Procurement and Transplantation Network in December, is meant to smooth out some of the regional differences in how sick a person has to become before getting a liver, said Anne Paschke, a spokeswoman for United Network for Organ Sharing, or UNOS, the Virginia-based nonprofit that runs the transplant network..
“What we’re looking at is saving as many lives as possible,” she said.
There will be winners and losers geographically. States like Missouri and Kansas, which have some of the highest organ donation rates in the country, are among the losers.
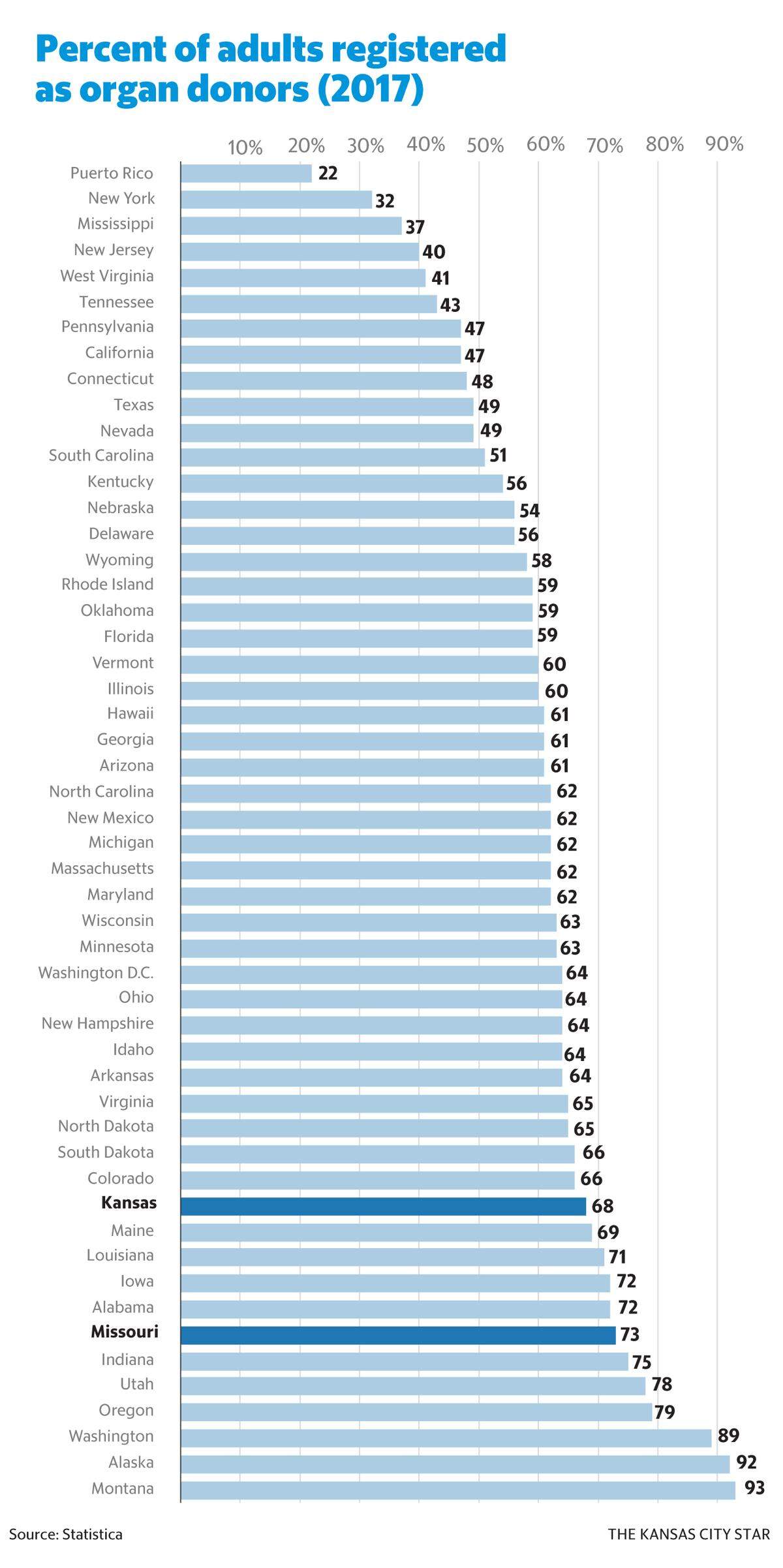
Paschke said computer models predict that the difference will be minimal and people in the Midwest who are ill will still have a better shot at getting a liver than people in most other parts of the country.
But that isn’t mollifying lawmakers.
Republican U.S. Sens. Roy Blunt of Missouri and Jerry Moran of Kansas recently criticized the change in a letter to the U.S. Department of Health and Human Services. That government agency contracts with the organ transplant network to operate the complicated donation web.
Moran and Blunt said the change is flawed because it unintentionally rewards regional organ donation groups that haven’t done as well at getting more organs or making sure available organs get used.
“This policy change does not appear to give any weight to locations that have been successful in reducing their wait lists through aggressive organ procurement or through adopting innovative transplant techniques,” the letter says. “Instead, the OPTN rewards locations that underutilize existing organ resources and have historically had troubled organ procurement organizations.”
Twenty other senators from Southern and Midwestern states co-signed the letter, including fellow Republicans Pat Roberts of Kansas and Josh Hawley of Missouri, as well as a few Democrats.
They worry that patients in their states will have to become far sicker before they can be eligible for a transplant.

“All I can say honestly is that I’m just happy I had my transplant prior to any change like that going through,” said Amy Ausmus of Lenexa, who received a new liver in 2017.
Ausmus, a single mom, was on the liver transplant list for about a year and a half, getting sicker and sicker. She was tired all the time, often bloated and nauseous and suffering the worst itching she could ever imagine.
She got her transplant at age 31, after almost a decade of dealing with ulcerative colitis and a bile duct condition called primary sclerosing cholangitis that caused her liver to fail.
“That was my normal, was just learning that something was always wrong every day,” Ausmus said. “So once I got my liver transplant and I recovered, I was actually taken aback by what it feels like to live pain-free and symptom-free from any diseases. I kept waiting for it to go back to the way I was used to and after a solid few weeks to a month of it not ever going back I was even more grateful but also still surprised, kind of like, ‘Wow, you know life is fun.’”
Moran’s office said the University of Kansas Hospital first brought concerns about the policy change to its attention. KU is one of three Kansas City-area hospitals with liver transplant programs, along with St. Luke’s and Children’s Mercy.
About 13,000 people are waiting for a liver transplant nationwide, yet only about 8,000 transplants were performed in 2018.
The way available livers have been allocated has been a matter of intense debate for years, pitting transplant centers in big cities, where more people are waiting, against those in more rural areas that have typically had more donors per capita. The reasons for the regional disparities are complex, but cultural differences and the quality of organ procurement programs are thought to play a role.
UNOS tweaked its liver distribution rules in late 2017 in an effort to reach a compromise. But a lawsuit filed in July by six patients from California, Massachusetts and New York spurred the larger overhaul that is coming in April.
Under the current distribution model, the sickest patients within 58 “Donor Service Areas” get first crack at livers that are donated in their area. Kansas City’s area includes all of Kansas and most of western Missouri.
Livers that aren’t claimed are then opened up to one of 11 geographic regions. Kansas City is in Region 8, which is made up of Colorado, Iowa, Kansas, Missouri, Nebraska and Wyoming.
The changes scrap that system in favor of a series of concentric circles drawn around the liver donation site. The sickest people within 150 miles get the first shot, followed by the sickest within 250 miles and then the sickest within 500 miles, regardless of state boundaries. In some cases, critically ill people may even be allowed a chance at a liver from more than 500 miles away.
That means livers that are donated in the Kansas City area might end up being shipped to Chicago, Dallas or the Mayo Clinic in Rochester, Minn. But most wouldn’t end up on the coasts, which suffer the most critical shortages.
Paschke said sick patients in Kansas City will still have a good shot at a transplant, compared to those in other parts of the country.
People on the liver transplant waiting list are assigned a “model for end-stage liver disease” or “MELD” score: a number between 6 and 40 that characterizes how ill they are based on a number of different tests. Forty is the most sick.
Computer modeling done by the transplant network predicts that the median score at transplant for people in Kansas City’s donor service area will rise from 25 to 29.4 after the changes. But that’s still lower than the projections for all but eight of the 58 donor areas. If the projections prove true, the only places in the country that will be significantly lower than Kansas City are Puerto Rico (21.4) and Hawaii (23), which are insulated by their island geography.
Still, the difference between 25 and 29.4 is not nothing. Ausmus said her MELD score fluctuated between about 20 and 30 for much of her time on the waiting list. It was 33 when she got her transplant.
“When it would move from a 25 to a 30 or 31, I definitely felt that,” Ausmus said. “It was more severe. I could sleep all day and yet still be tired.”
Ausmus had moved to Kansas from California four years before her transplant, a move she now says may have saved her life.
“Even though my MELD was only 33, that doesn’t mean that I wasn’t going to lose my life waiting on the transplant list,” Ausmus said. “MELD 33 may be lower than other states that are at 40, but my 33 could have taken my life in the next three months.”
But Julie Heimbach, a Mayo Clinic physician who chairs the transplant network’s liver and intestine committee, said the current system was not designed to optimally distribute livers, and the coming system will be more fair to patients nationwide.
“It doesn’t matter where they are, they should have an equal chance at a transplant,” Heimbach said.
She said she agreed that some regional organ procurement organizations have been better at convincing people to donate their organs than others, but the patients waiting for transplants have no control over that.
The key to getting a liver for everyone who needs one, she said, is increasing donations throughout the country. In the meantime, she said, the new system will do a better job of getting the sickest people to the front of the line.
KU Hospital disagreed with that in a letter to her committee that was also signed by Barnes-Jewish Hospital in St. Louis and Vanderbilt University Medical Center in Nashville.
The letter said the new system is projected to slightly decrease the total number of transplants nationwide because longer travel times will increase the possibility of organs being wasted. The hospitals said that the committee relied too much on the MELD score and that the policy was “hastily cobble(d) together” because of the lawsuit in a way that was “legally untenable.”
“None of the proposed models complies with the law and any policy development process must include proper consideration of socioeconomic inequities and access to transplantation, including the waiting list, for all end-stage liver disease patients,” the hospitals wrote.
Hospital officials urged the organ transplant network to take “a phased approach” to implementing the changes and regularly evaluate whether they prove harmful to people of lower socioeconomic status and how they affect access to care, organ wasting and the overall volume of transplants.
Heimbach said she completely agreed with that.
“At the end of the day, it’s a hard change and a big change,” Heimbach said. “Everything we do will have to be closely monitored to make sure it’s meeting the goals of the program.”
This story was originally published February 3, 2019 at 5:30 AM with the headline "Bigger cities face organ donation shortage. So they plan to take them from KC area."
